In this section you can find research activities, scientific projects and theses for bachelor’s, master’s, doctoral or postgraduate degrees, curated and promoted by CiaoLapo ETS Foundation.
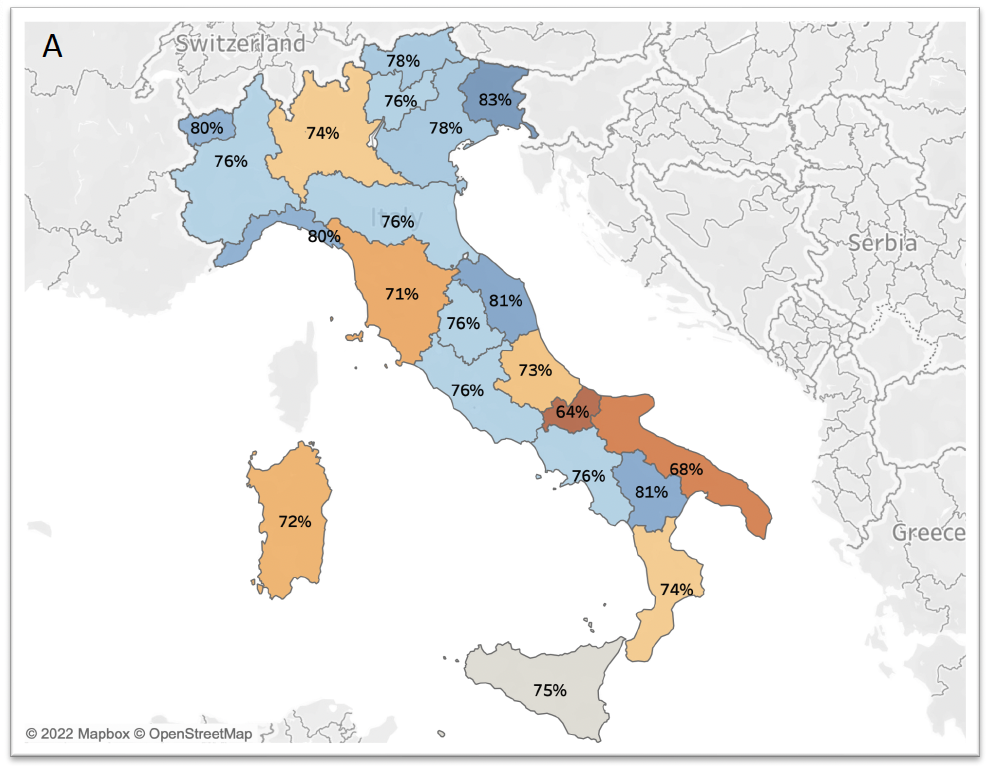
The LISTEN (Lactation Support afTer pEriNatal loss) study closed in December 2023 with the participation of 1227 health care providers involved in perinatal bereavement care, distributed throughout the country. The results were published on December 23, 2025 in the Journal of Midwifery & Women’s Health with the title. “The LISTEN (Lactation Support afTer pEriNatal loss) Project: Pathways of Loss and Lactation Care in Italy”, authored by Claudia Ravaldi, Laura Mosconi, Alfredo Vannacci and a group of colleagues from the Universities of Florence, Verona, Parma, Tor Vergata in Rome and Politecnica delle Marche, in collaboration with CiaoLapo Foundation.
This is the first Italian study specifically dedicated to the management of lactation after perinatal loss, a topic that, despite having important clinical, emotional and relational implications, has long remained on the margins of both guidelines and practitioner training. Indeed, the physiological onset of breastfeeding after the death of an expected or newly born child confronts the woman with suffering that is not only physical, and requires informed, respectful, and individualized care. The available options (pharmacological suppression, physiological suppression, milk donation) have different meanings and implications, and the choice should always arise from a process of shared decision making, based on complete and timely information.
The champion
The sample is overwhelmingly composed of women (97.5 percent) and midwives (76.8 percent), followed by nurses (12.8 percent), physicians (6.6 percent), psychologists (1.6 percent) and other professionals. About half of the providers (51.4 percent) have less than 10 years of experience, and 80.2 percent work in public hospitals, mainly in delivery rooms and maternity wards. More than half of the sample has directly witnessed cases of endouterine death (69.7%) or neonatal death (53.1%).
Training and guidelines: a first paradox
A first finding from reading the results is the discrepancy between the training received and the organization of the departments. 60.2% of providers have attended specific training on perinatal bereavement, and rated its usefulness very highly (4.7 out of 5). However, only 42.5 percent report having a formalized guideline for perinatal bereavement care in their workplace, and only 31.5 percent report the existence of a structured psychological support course for parents. Of those who indicate the presence of a guideline, 33.3 percent do not know exactly how long it has been in place. The perceived usefulness of a guideline, in the words of respondents, is very high (4.8 out of 5): the problem, therefore, is not the willingness of practitioners to apply it, but the widespread absence of an institutional framework.
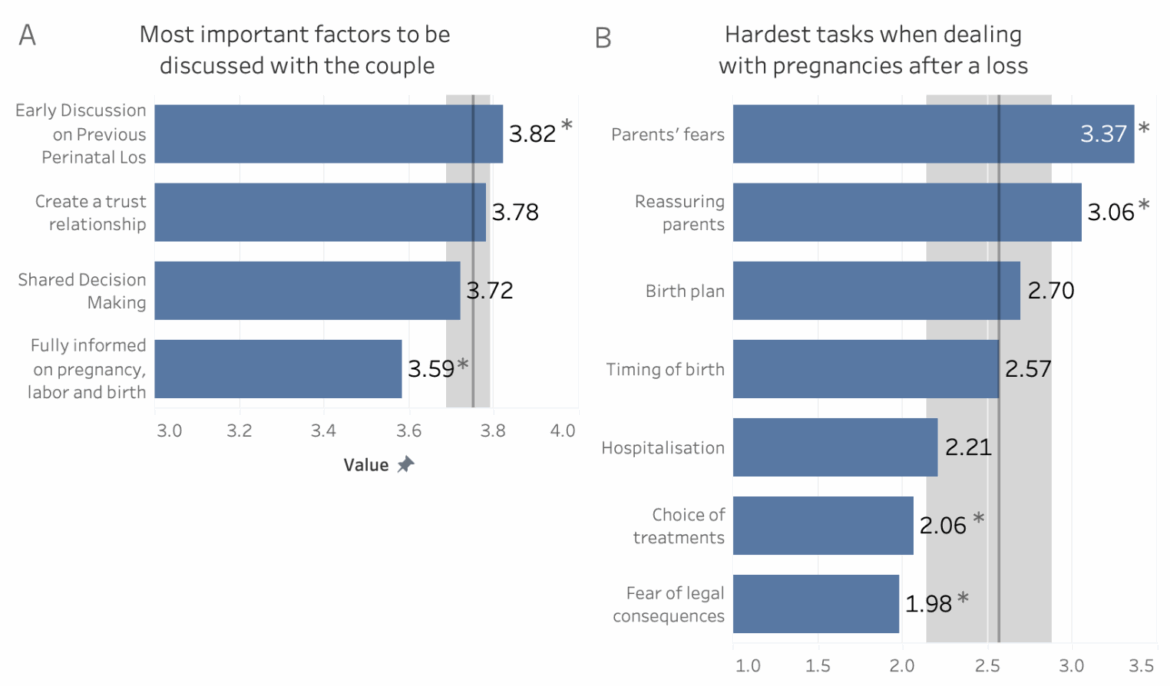
The management of perinatal bereavement is described as emotionally very strenuous in both scenarios studied (7.7 out of 10 for endouterine death, 7.8 out of 10 for neonatal death), while the clinical difficulty is slightly greater in cases of neonatal death than in utero death (5.3 vs. 4.9). Practitioners who have undergone specific training report slightly less emotional distress, a finding in line with what has already been observed in the CLASS, BLOSSoM and STRONG studies, which have shown the protective role of training with respect to burnout and post-traumatic symptoms.
Lactation after a loss: an area still opaque
The core of the LISTEN study concerns lactation management after loss. Practitioners attribute a modest level of training on lactation suppression techniques to themselves (average 2.7 out of 5). About a quarter of the sample reports that they did not provide any information on lactation management even though they had the opportunity to do so: some did not know what to say, some had never thought about the topic, and a significant proportion (9.6 percent in cases of endouterine death and 8.4 percent in cases of neonatal death, for a total of 78 practitioners) do not consider lactation counseling as part of their professional responsibilities. The latter position is more frequent among physicians (13.6 percent) and psychologists (10.0 percent) and less frequent among nurses (7.6 percent) and midwives (5.6 percent).
On the choice of the most appropriate time to talk about lactation, 64.7 percent of practitioners believe it is correct to do so within 24 hours of delivery, 12.2 percent before delivery, 10.4 percent immediately after, while 7.8 percent address the topic only if the woman asks for it. Instead, international guidelines recommend that the information be offered at the time of diagnosis to ensure that the woman has time to make an informed choice.
As for the type of information provided, the clearest finding is the absolute prevalence of pharmacological suppression: it is discussed in 89.5 percent of cases of endouterine death and 83.8 percent of cases of neonatal death. Complications (engorgement, mastitis, milk loss) are addressed by about 62% of respondents. Milk donation, on the other hand, is proposed by only 21.8% of providers after an endouterine death and 25.4% after a neonatal death, a very low proportion considering that Italy is the European country with the largest number of donated human milk banks. The gap between the availability of resources and the actual provision of information to families suggests that the critical issue is cultural and educational, not logistical.
On the effectiveness of different lactation management strategies,manual expression is the one considered most useful by respondents, while compression bandages are judged to be ineffective, consistent with the international literature, which does not recognize evidence to support nonpharmacological interventions when compared with nonintervention. Pharmacological therapy remains, to date, the only evidence-based approach to be offered along with the possibility of milk donation according to a shared choice model.
Written information to be delivered to the woman at discharge is almost absent: only 15.8% of operators report that they deliver dedicated information material, although they consider it useful. Finally, post-discharge follow-up is described as lacking by 78.2 percent of the sample: only 21.8 percent of operators report the existence of a structured follow-up pathway, and only 28.1 percent know of a dedicated outpatient service in their area.
The voices of the operators
The study also included a qualitative analysis of open-ended questions, which were answered by 76.2 percent of the sample. Recurring themes emerged from the responses, with which CiaoLapo operators are familiar from their daily experience: the centrality of communication, the difficulty of finding words, the need for empathy while maintaining a professional boundary, the sharing of grief, the sense of helplessness, bureaucratic obstacles and, specifically in cases of endouterine death, silence as a symbol of absence and the social taboo that still surrounds these events. Many practitioners report, in responding to the questionnaire, that they are reflecting for the first time in a structured way on lactation after loss, and they ask for protocols, continuing education and psychological support for themselves.
What LISTEN tells us, and where our work is going
LISTEN’s results confirm some of the hypotheses that have guided the Foundation’s work for years, and add new ones.
The first element is that specific training works: where it is there, emotional difficulties are alleviated and the quality of care reported increases. The second is that training alone is not enough: without formalized workplace guidelines, and without structured pathways for psychological support and follow-up, even the best-trained providers operate in clinical solitude. The publication in February 2023 of the National Recommendations on the Management of Fetal Endouterine Death, to whose drafting the Foundation contributed, is a first step in this direction, but the document, as the authors themselves acknowledge, devotes limited attention to lactation management: the LISTEN data suggest that this gap needs to be filled.
The third element concerns milk donation. The gap between the Italian network of donated human milk banks and the actual proposal of this option to bereaved women indicates that there is a wide educational and cultural space, on which the Foundation intends to work in the coming years in continuity with its research and training activities, including through the PeaRL Laboratory at the University of Florence.
Finally, the fourth element is the one that respondents themselves expressed most clearly: continuity of care, from diagnosis to territorial follow-up, cannot be considered an optional addition. It is a constitutive part of respectful care, and its absence is today, in Italy, one of the most urgent issues to be addressed.